In medical billing, understanding the difference between referrals and authorizations is necessary. A referral is when your primary care doctor sends you to a specialist for further care. An authorization is permission from your insurance company to cover a specific service or treatment.
Both processes help make sure that patients receive the right care while testing costs manageable. But, if either step is missed, it can lead to claim denials and unexpected bills. In this we will explore seven key insights about referrals and authorizations to help you steer the healthcare system more effectively.
Key Takeaways
- Authorization is permission from the insurance company for specific medical services, while a referral is a recommendation from a primary care provider to see a specialist.
- Understanding the distinction between referrals and authorizations is critical to avoid claim denials and make sure proper patient care.
- Referrals are often required by Health Maintenance Organizations (HMOs) to coordinate care within a network, while authorizations are needed for certain high-cost services.
- Errors in obtaining referrals or authorizations can lead to significant delays and increased out-of-pocket costs for patients.
- Staying informed about changing payer rules and documentation standards is necessary for healthcare providers to optimize billing practices and prevent denials.
Definition of Referral in Medical Billing

In medical billing, a referral is a formal recommendation from a primary care provider (PCP) for a patient to see a specialist. This process ensures that patients receive the right care tailored to their specific needs. Referrals are significant for coordinating patient care and are often required by insurance plans, especially Health Maintenance Organizations (HMOs). Without a valid referral, patients may face claims denials when seeking treatment from specialists.
It is vital to understand the difference between a referral and authorization. A referral directs patients to specialists, while authorization is the insurance company’s approval for specific services or treatments. For instance, before a patient undergoes surgery, their healthcare provider must obtain prior authorization to confirm that the procedure is medically necessary and covered by the patient’s insurance policy.
Both referrals and authorizations are key parts of the reimbursement process. They help manage costs and make sure compliance with healthcare regulations. By following these procedures, healthcare providers can reduce claim denials and improve patient care.
| Referral | Authorization |
|---|---|
| Recommendation from PCP to see a specialist | Insurance approval for specific services |
| Required by many insurance plans | Necessary for certain high-cost procedures |
Definition of Authorization in Medical Billing

In medical billing, authorization is the process where an insurance company gives permission for a specific medical service or treatment. This step is significant since it confirms that the service is necessary and covered by the patient’s insurance policy. Without proper authorization, claims may be denied, which can lead to unexpected costs for patients.
A referral is different. It is a recommendation from a primary care provider (PCP) for a patient to see a specialist. Referrals help coordinate care and make sure patients get the right treatment. While both processes are critical for patient care, they have different roles in the healthcare system.
Knowing the differences between authorization and referral can greatly affect the reimbursement process and help prevent claim denials. For instance, if a patient visits a specialist without the necessary referral or authorization, the insurance may not cover the costs, leaving the patient responsible for the bill.
| Aspect | Authorization | Referral |
|---|---|---|
| Definition | Insurance approval for services | Doctor’s recommendation to a specialist |
| Who Issues It? | Insurance Company | Primary Care Provider (PCP) |
| Impact on Claims | Required for payment | Facilitates specialist visits |
Key Differences Between Referral and Authorization
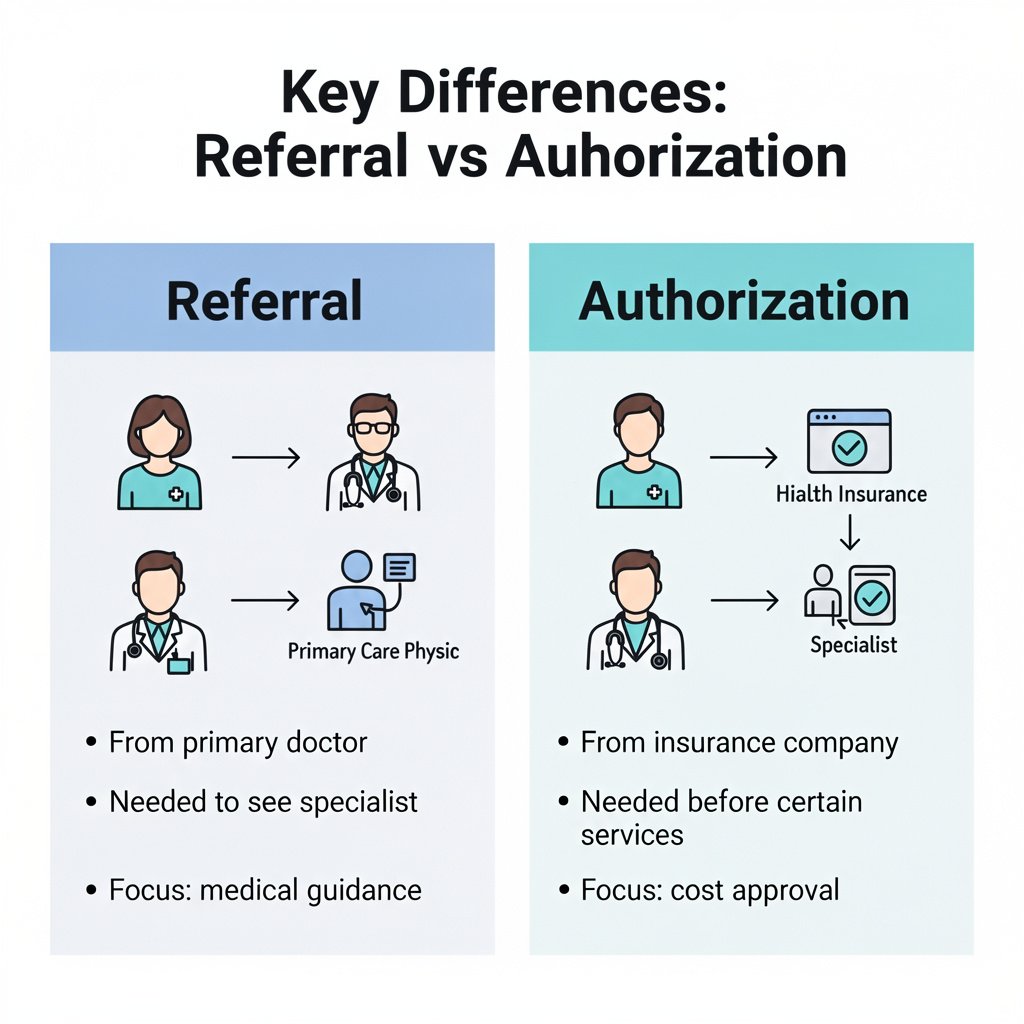
In medical billing, knowing the differences between referrals and authorizations is significant. Both play a key role in making sure patients get the right insurance coverage and effective patient care.
Referrals are recommendations from a primary care provider (PCP) for a patient to visit a specialist. This process helps make sure that patients receive the right care for their health issues. For example, if someone needs to see a cardiologist, their PCP will provide a referral.
Authorizations are permissions given by the insurance company before a specific service can be performed. This step is critical for confirming that the treatment is necessary and covered by the patient’s plan. For instance, a patient may need prior authorization for an MRI.
Here’s a quick comparison:
| Aspect | Referral | Authorization |
|---|---|---|
| Issued By | PCP | Insurance Company |
| Purpose | Directs to a specialist | Confirms medical necessity |
| Required For | Specialist visits | Certain treatments |
Understanding these differences can help prevent claims denials and make sure a smoother reimbursement process.
Importance of Referrals in Patient Care

Referrals play a critical role in patient care, acting as a link between primary care providers and specialists. When a primary care physician (PCP) sees the need for specialized treatment, they issue a referral. This process ensures that patients receive the expert care they need for their conditions. Without a proper referral, patients might face insurance claim denials, which can lead to unexpected costs.
On the flip side, authorizations are permissions obtained from insurance companies before certain services are provided. This step confirms that the treatment is medically necessary and covered by the patient’s insurance plan. Both referrals and authorizations are necessary for smooth healthcare delivery and reimbursement.
Understanding the differences between referrals and authorizations can greatly impact patient care and financial outcomes. For example:
- Referrals: Initiated by a PCP to guide patients to specialists.
- Authorizations: Required by insurers to approve specific treatments.
By mastering these concepts, healthcare providers can improve patient care coordination and reduce claims denials.
Importance of Authorizations in Insurance Claims

Understanding the importance of authorizations in insurance claims is key to effective healthcare delivery. An authorization is a formal approval from an insurance company that allows a healthcare provider to perform a specific service. This process ensures that the treatment is considered medically necessary and covered by the patient’s insurance plan.
A referral, conversely, is a recommendation from a primary care provider (PCP) for a patient to see a specialist. While both authorizations and referrals are significant, they serve different purposes. Authorizations help prevent unnecessary costs and make sure compliance with payer requirements, while referrals guide patients to the right care.
- Claims Denial Prevention: Without proper authorization, claims may be denied, leading to unexpected out-of-pocket expenses.
- Cost Containment: Authorizations help control healthcare costs by ensuring only necessary services are provided.
- Streamlined Care: Efficient authorization processes improve patient care by reducing delays in treatment.
In short, understanding the roles of authorizations and referrals is critical for finding your way the healthcare system. This knowledge not only helps secure necessary treatments but also reduces the risk of claim denials, ensuring a smoother reimbursement process. For more information on this topic, visit healthcare authorizations.
Common Challenges in the Referral Process
In the referral process, we often face challenges that can make patient care and billing more complicated. Understanding these challenges is significant for both healthcare providers and patients. Here are some common issues:
- Miscommunication: Sometimes, the details of referrals are not clearly shared between the primary care provider (PCP) and the specialist. This can lead to confusion about what the patient really needs.
- Insurance Requirements: Different insurance plans have different rules for referrals. Not knowing these rules can result in claim denials.
- Documentation Errors: If clinical documents are incomplete or incorrect, it can slow down the referral process and affect payments.
- Eligibility Verification: Not checking a patient’s eligibility for services can lead to unexpected costs that they have to pay out of pocket.
To overcome these challenges, we need to make sure clear communication, understand insurance requirements, and keep accurate documentation. This proactive approach helps make the referral process smoother, which improves patient care and reduces claim denials.
| Challenge | Impact |
|---|---|
| Miscommunication | Leads to unclear patient needs |
| Insurance Requirements | Results in claim denials |
| Documentation Errors | Hinders referral and reimbursement |
| Eligibility Verification | Causes unexpected costs for patients |
Common Challenges in the Authorization Process
In the medical billing process, challenges often arise during the authorization phase. This phase is necessary for making sure healthcare providers get paid for the services they provide. Here are some common challenges we face:
- Complex Payer Requirements: Each insurance company has its own rules about prior authorizations, which can create confusion and delays.
- Documentation Errors: Mistakes in clinical documentation can lead to claim denials, affecting the reimbursement process.
- Time Constraints: The authorization process can take a long time, causing delays in patient care and increasing the workload for staff.
- Communication Gaps: Miscommunication between healthcare providers and insurance companies can result in misunderstandings about what services are covered.
To handle these challenges effectively, we must focus on clear communication and careful documentation. Understanding the differences between referrals and authorizations is key to reducing claim denials and ensuring compliance with healthcare regulations.
| Challenge | Impact |
|---|---|
| Complex Payer Requirements | Delays in authorization and payment |
| Documentation Errors | Increased claim denials |
| Time Constraints | Delayed patient care |
| Communication Gaps | Misunderstandings about coverage |
Impact of Referrals on Claims Denial Rates
Understanding how referrals affect claims denial rates is significant in medical billing. Referrals are recommendations from a primary care provider (PCP) to see a specialist. They help make sure patients get the care they need. But, if these referrals are not properly authorized, they can lead to claims denials.
Here’s how it works:
- Referral Process: A PCP sees that a patient needs specialist care and issues a referral.
- Authorization Requirement: Many insurance plans need prior authorization for certain services, even with a referral.
- Claims Denial Risk: If a referral is not authorized, the insurance may deny the claim, leaving patients to pay the costs.
To reduce claims denials, we must make sure that referrals come with the necessary authorizations. This means understanding payer requirements and testing clear communication between healthcare providers and patients.
| Referral Status | Claims Outcome |
|---|---|
| Authorized Referral | Claim Approved |
| Unauthorized Referral | Claim Denied |
By understanding these processes, we can improve patient care and lower unnecessary costs linked to claims denials.
Impact of Authorizations on Reimbursement Process
In medical billing, understanding how authorizations affect the reimbursement process is very significant. Authorizations are permissions given by insurance companies before a patient gets specific services. This step makes sure that the treatment is medically necessary and covered by the patient’s insurance plan. Without the right authorization, claims can be denied, which can lead to unexpected costs for both patients and providers.
A referral, conversely, is a recommendation from a primary care provider (PCP) to see a specialist. While referrals help guide patient care, they do not guarantee that the insurance will pay for the service. Both authorizations and referrals are key for smooth claims processing and avoiding claims denials.
Here’s a quick comparison:
| Aspect | Authorization | Referral |
|---|---|---|
| Purpose | Insurance approval for services | Recommendation to see a specialist |
| Who Issues? | Insurance company | Primary care provider |
| Impact on Payment | Critical for reimbursement | Helps make sure coverage |
By understanding these differences, we can steer the complexities of healthcare more effectively. This knowledge helps make sure that patients receive the care they need while minimizing financial surprises. For more information on authorizations, check out this resource.
Best Practices for Managing Referrals and Authorizations
In medical billing, managing referrals and authorizations is critical for ensuring patient care and securing insurance coverage. Understanding the difference between these two processes can greatly reduce claim denials and improve the reimbursement process.
Referrals are recommendations from a primary care provider (PCP) for patients to see specialists. They help patients get the right care while following insurance policies. Conversely, authorizations are permissions obtained from insurance companies before certain services are provided. These confirm that the service is necessary and covered.
To steer these processes effectively, follow these best practices:
- Verify Eligibility: Always check the patient’s insurance coverage and provider network before starting referrals or authorizations.
- Document Thoroughly: Keep clear clinical documentation to support the medical necessity of referrals and authorizations.
- Communicate Clearly: Make sure that everyone involved—patients, providers, and insurers—understands the requirements and processes.
- Track Progress: Monitor the status of referrals and authorizations to prevent delays in patient care.
By using these strategies, we can improve patient experiences and streamline the billing process, leading to better healthcare outcomes.
People Also Ask (FAQs)
No. A referral comes from a PCP; authorization comes from the payer.
Yes. Specialist visits may only need referrals, not PA.
Yes. Imaging tests or surgeries may require PA only.
Insurance denies the claim. The patient may be responsible for the full amount.
The provider performing the service—not the patient.
Conclusion
Understanding the difference between referrals and authorizations is critical for effective medical billing. Referrals guide patients to specialists, while authorizations make sure insurance coverage for treatments. Both processes are critical in preventing claim denials and ensuring smooth patient care. By grasping these concepts, we can improve our billing practices and improve patient experiences. Staying informed about changing payer rules and documentation standards will help us steer the complexities of healthcare more effectively. Let’s prioritize clear communication and proper procedures to optimize our practice’s financial health and patient satisfaction.
